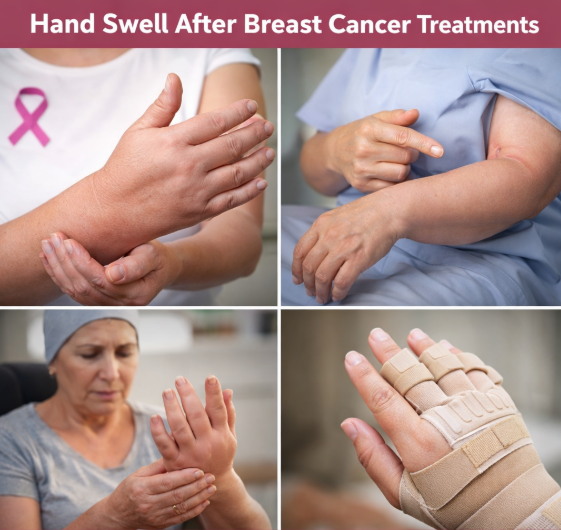
If your hand or arm is swelling after breast cancer treatment, you’re not alone and you’re not overthinking it. In Kathmandu Valley (Kathmandu, Lalitpur, Bhaktapur), many patients notice swelling weeks, months, or even years after surgery or radiation. The most common cause is breast cancer related lymphedema, but swelling can also come from infection, vein clots, inflammation, or scar-related circulation changes. This guide explains the real reasons, the red flags you must not ignore, and a clear plan to reduce swelling safely based on how breast cancer care is actually delivered in Nepal.
Dr. Kapendra Shekhar Amatya, a leading Breast Cancer surgeon in Nepal, has 20+ years of surgical oncology experience and is known for breast conserving and reconstructive approaches that prioritize both cancer control and long-term function.
Direct definition
Hand swelling after breast cancer treatment is most often due to lymphedema a buildup of lymph fluid when lymph vessels or nodes are damaged by surgery or radiation. It can cause heaviness, tightness, swelling, and reduced movement. Early detection and structured management can significantly control symptoms and reduce complications.
The direct answer: Why does the hand swell after breast cancer treatment?
Most commonly, swelling happens because the lymph drainage system on the treated side has been disruptedespecially after axillary lymph node surgery or radiation. That disruption makes fluid collect in the arm/hand over time, leading to visible swelling and a “full” or heavy feeling.
But not all swelling is lymphedema. Some causes require urgent evaluation, so the next section helps you differentiate quickly.
Hand/arm swelling after breast cancer: what it usually means (and what it could mean)
Quick comparison table (save this)
| Cause | What it feels/looks like | Timing | Risk level | What to do |
|---|---|---|---|---|
| Lymphedema (most common) | Gradual swelling, heaviness, tightness; may worsen by day end | Weeks to years later | Moderate (manageable, chronic) | Early assessment + compression + therapy |
| Infection (cellulitis) | Redness, warmth, tenderness; may have fever | Anytime; often sudden | High | Same-day medical review |
| Blood clot (DVT) | Sudden swelling, pain, color change; sometimes shortness of breath | Sudden | High | Emergency evaluation |
| Post-surgery inflammation/seroma effects | Localized swelling near surgery/underarm, stiffness | Early weeks | Variable | Surgeon follow-up |
| Radiation fibrosis / scarring | Tightness, reduced mobility, swelling with stiffness | Months later | Moderate | Rehab + targeted therapy |
| Cancer recurrence (less common) | Persistent swelling + new lumps, pain, weight loss, new symptoms | Later | High | Prompt oncologic evaluation |
Red flags (don’t wait):
- Sudden swelling over hours–1–2 days
- Fever, redness, warmth, worsening pain
- Shortness of breath or chest pain
- Rapidly worsening swelling with severe heaviness
These require urgent medical assessment to rule out infection or clot.
Why breast cancer treatments trigger swelling (the “LYMPH” pathway)
1) Lymph nodes act like drainage checkpoints
Your arm and hand have lymph vessels that drain fluid through lymph nodes, many of which sit in the underarm (axilla).
2) Surgery can reduce drainage capacity
Procedures that may increase risk include:
- Sentinel lymph node biopsy (SLNB) (lower risk)
- Axillary lymph node dissection (ALND) (higher risk)
When lymph ducts/nodes are disrupted, lymph can’t flow as efficiently, leading to swelling.
3) Radiation can stiffen lymph channels and surrounding tissues
Radiation can cause tissue changes that reduce lymph flow and increase swelling risk over time.
4) “Trigger events” can tip a stable arm into swelling
Even after healing, swelling may appear after:
- Infection, minor cuts, burns
- Weight gain
- Overuse without gradual conditioning
- Long travel or prolonged immobility
Quotable expert-style statement: “Lymphedema isn’t only about what was removed it’s about how much drainage capacity remains versus how much fluid load the arm must handle every day.”
Section summary (extractable)
- Surgery + nodes and radiation reduce drainage capacity
- Triggers (infection, strain, weight changes) increase fluid load
- Lymphedema appears when load > capacity
Is it lymphedema? A practical self-check (and when to confirm clinically)
Common early symptoms (Stage 0–1 patterns)
You may notice:
- Rings feel tight, bangles don’t fit
- Sleeve feels tighter on one side
- Heaviness, fullness, or tightness (even before visible swelling)
- Mild swelling that improves overnight
NCCN patient guidance highlights that subtle swelling/heaviness should be reported early because early stages are more reversible.
Simple “3-point check” you can do safely
- Compare both hands in the morning and evening
- Notice jewelry tightness changes
- Look for persistent “sock-line” type indentations on the swollen hand/forearm
How clinicians confirm (what to expect in Kathmandu Valley)
Depending on availability, confirmation may include:
- Limb circumference measurements at fixed points
- Clinical staging and history
- Bioimpedance or volume tools where available
- Rule-outs if red flags exist (e.g., clot/infection evaluation)
The International Society of Lymphology (ISL) consensus emphasizes structured diagnosis and staging for peripheral lymphedema.
The step-by-step plan: reduce swelling safely (without guesswork)
Step 1: Rule out urgent causes first
If swelling is sudden, painful, hot/red, or accompanied by fever/breathlessness seek urgent care.
Step 2: Get a baseline assessment (so you can track progress)
Ask your breast team to document:
- Side involved (treated side vs both)
- Measurement points
- Skin condition (dryness, cracks, infection risk)
- Shoulder/arm range of motion
Step 3: Start evidence-aligned first-line management
Most guideline-aligned pathways include complete decongestive therapy (CDT) principles:
- Compression (sleeves/garments as advised)
- Manual lymphatic drainage by trained therapists
- Exercise (graded and specific)
- Skin care to prevent infection
Step 4: Build a “maintenance routine” (the part that keeps results)
Once swelling reduces, long-term control relies on:
- Consistent compression use as prescribed
- Ongoing movement and strengthening
- Weight management and infection prevention
Step 5: Consider surgical options only when appropriate
For select patients with persistent swelling, specialized microsurgical procedures may be considered in advanced centers, but they’re not the first step for most people. (Discuss candidacy with your surgical oncologist and a lymphedema-focused team.)
Section summary
- First: rule out infection/clot
- Then: measure + stage + start CDT basics
- Finally: maintain and reassess periodically
What helps at home (safe) vs what can worsen swelling
Helpful, generally safe practices (when no red flags)
- Keep the arm moving gently: wrist circles, open/close fist, elbow flex/extend
- Elevate occasionally (not as the only strategy)
- Moisturize skin; treat cracks early
- Protect from cuts, burns, insect bites
- Gradual strength training (not sudden overload) when cleared
NCCN patient survivorship guidance supports early reporting and structured management rather than “wait and see.”
Things that often worsen swelling
- Ignoring early tightness until swelling becomes obvious
- Unsupervised aggressive massage (wrong direction/pressure)
- Sudden intense exercise after long inactivity
- Repeated needle sticks or injuries on the affected arm (when avoidable)
- Heat extremes (hot packs/sauna) if you notice they trigger swelling
Quotable expert-style statement: “The goal isn’t to ‘rest’ the arm forever the goal is to train the arm to handle daily load with the right protection.”
The “ARM SAFE” prevention framework (original, practical, cite-friendly)
Use this after breast surgery/radiation to reduce long-term risk:
A — Assess early: baseline measurement + early symptom reporting
R — Reduce infection risk: skin care, treat cuts, avoid untreated fungal infections
M — Move daily: gentle mobility + gradual strengthening
S — Sleeve when indicated: compression during high-load days/travel (if prescribed)
A — Avoid sudden overload: increase weights/chores gradually
F — Fit matters: properly fitted garments, bras, and prosthetics
E — Engage follow-up: periodic check-ins (especially first 2 years)
This aligns with core principles emphasized in consensus and survivorship guidance: early detection + structured management.
Why choosing the right specialist in Nepal matters
Hand swelling isn’t just a symptom it affects work, sleep, confidence, and long-term arm function. A breast doctor in Nepal who understands both cancer control and survivorship can:
- Choose lymph-node approaches appropriately (when clinically safe)
- Coordinate rehab early (not after swelling becomes severe)
- Protect long-term function alongside cosmetic outcomes (oncoplastic planning)

Dr. Kapendra Shekhar Amatya is presented on his official site as a senior surgical oncologist with 20+ years of experience, with emphasis on breast-conserving surgery, reconstruction, and multidisciplinary care important for reducing long-term functional complications.
FAQ (optimized for featured snippets + voice search)
1) Why does my hand swell after a mastectomy or lumpectomy?
Most often due to lymphedema, where lymph fluid builds up because lymph nodes/vessels were affected by surgery or radiation. It can start subtly with tightness and heaviness before visible swelling.
2) Can hand swelling start years after breast cancer treatment?
Yes. Lymphedema can appear months or years later, especially after triggers like infection, weight gain, or increased arm strain.
3) Is lymphedema dangerous?
It’s usually manageable, but it can raise infection risk and worsen without treatment. Early-stage detection and therapy can prevent progression and improve quality of life.
4) What are the warning signs that swelling is an emergency?
Sudden swelling, redness/warmth, fever, severe pain, or breathing difficulty needs urgent evaluation to rule out infection or blood clot.
5) What is the best treatment for breast cancer–related lymphedema?
First-line care often includes compression, manual lymph drainage by trained providers, exercise, and skin care (CDT principles), tailored to your stage and symptoms.
6) Will exercise make lymphedema worse?
Appropriately graded exercise is generally helpful and supports function. Problems usually come from sudden overload without a plan.
7) Can a breast cancer surgeon help with swelling problems?
Yes, your Breast Cancer surgeon in Nepal coordinates survivorship care, rules out surgical causes, and connects you with rehab/lymphedema therapy when needed especially important early.
8) How do I choose a breast cancer doctor in Nepal for survivorship issues?
Look for clear staging/treatment documentation, rehabilitation coordination, and experience in modern breast surgery approaches. Dr. Kapendra’s site highlights long-term experience and multidisciplinary focus.
Actionable conclusion (what to do next)
If your hand is swelling after breast cancer treatment, don’t guess.
Do this in order:
- Check red flags (sudden swelling, fever, redness, breathing issues) → urgent care
- Schedule assessment with a breast cancer doctor in Nepal (measure + stage)
- Start structured management early (compression/therapy/exercise/skin care)
- Use ARM SAFE prevention to reduce flare-ups
If you’re in Kathmandu, Lalitpur, or Bhaktapur, consider consulting Dr. Kapendra Shekhar Amatya, a senior breast surgical oncologist with 20+ years of experience as described on his official website, for a personalized evaluation and survivorship plan.
Educational note: This article supports awareness and planning; it doesn’t replace individualized medical care.


